New study reveals inequities in healthcare access and quality
Published June 8, 2017
A new analysis by Global Burden of Disease collaborators highlights that people are still dying from preventable, treatable causes, and reveals inequitable global progress in improving healthcare access and quality. Published in the Lancet on May 18, 2017, the study, “Healthcare Access and Quality Index based on mortality from causes amenable to personal health care in 195 countries and territories, 1990–2015: a novel analysis from the Global Burden of Disease Study 2015” has already garnered global attention.
New #GBDstudy ranks health care access and quality for 195 countries, according to 32 diseases - paper at: https://t.co/4dOhP9EMKZ @IHME_UW pic.twitter.com/IKRrB8Wxas
— The Lancet (@TheLancet) May 19, 2017
Using results from the Global Burden of Disease study, led by the Institute for Health Metrics and Evaluation (IHME), researchers analyzed 32 causes of disease and injury that should not be fatal if an individual has access to high-quality healthcare. The result is a new metric, the Healthcare Access and Quality Index (HAQ), a 0 to 100 scale that quantifies levels of personal access and quality of healthcare service delivery in 195 countries and territories across the globe.
Media sources including The New York Times, Fortune, Bloomberg, and BuzzFeed have covered the results from the paper, emphasizing where the US has fallen short on healthcare in comparison to other high-income countries, like Canada. “Americans pay too much for their health care and are among the sickest people in the developed world,” wrote Peter Aldhous from BuzzFeed.
Meanwhile, The Times has called out the UK for lagging behind its European counterparts, such as Finland, Sweden, Spain, and Italy, when it comes to quality healthcare, ranking 30th out of the 195 countries on the HAQ Index spectrum.
Map of HAQ Index values, by decile, in 1990 (top) versus 2015 (bottom)
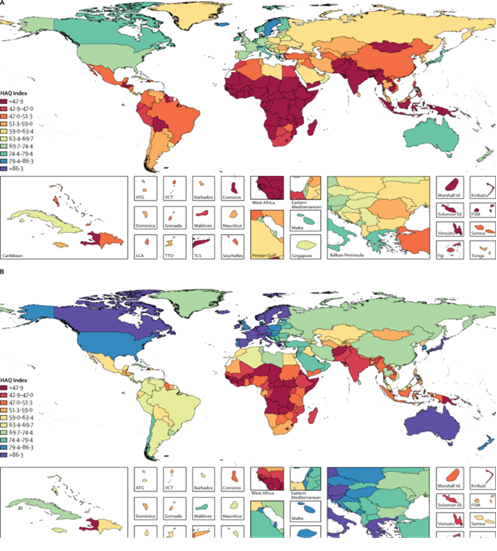
Analysis of HAQ index values reveals a general improvement in healthcare access and quality since 1990, with 167 of 195 countries showing statistically significant increases in HAQ Index values. Countries like South Korea, Turkey, Peru, China, and the Maldives showed the largest increases in HAQ Index levels since 1990. However, the gap between lowest and highest HAQ Index levels is greater now than it was before.
Although HAQ Index values are predicted by geography and level of development, the study found an unexpected diversity in results. The authors suggest that healthcare access and quality also differ by health focus areas within countries. For example, countries that rank lower in development may perform better in areas of vaccine-preventable diseases and worse in cancer prevention or other more complex disease management areas. Additionally, the study compared countries to an optimal HAQ Index for their development level, finding that some countries showed higher-than-expected healthcare access and quality, while other countries showed suboptimal personal healthcare and access for their stage of development. In other words, even though countries have been getting richer, they are doing relatively worse at improving equitable access and quality of their healthcare.
“What we have found about healthcare access and quality is disturbing,” said Dr. Christopher Murray, senior author of the study and Director of the Institute for Health Metrics and Evaluation (IHME). “Having a strong economy does not guarantee good healthcare. Having great medical technology doesn’t either. We know this because people are not getting the care that should be expected for diseases with established treatments.”
Having already sparked global interest, results from this analysis are a reminder that development is not the only indicator of healthcare access and quality, and that improvements can occur more rapidly, particularly in countries that are lagging behind. The new HAQ Index will help countries from all levels of development target areas where they can improve their healthcare service delivery, and inspire global efforts to improve equity in healthcare access and quality.